What is cirrhosis?
Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases.
Common causes of cirrhosis include:
- Long-term alcohol abuse.
- Chronic viral hepatitis (hepatitis B or C).
- Nonalcoholic fatty liver disease (NAFLD)
- Hemochromatosis.
The liver is one of the most important organs in your body and weighs about three pounds. It sits in the upper-right side of the abdomen, below the ribs.
The functions of the liver include:
- Changing food into energy.
- Cleaning out your body (metabolizing, or helping your body use, medications and removing alcohol and poisons from your system).
- Making bile. (Bile is a yellow-brown liquid made by the liver from bile salts, cholesterol, bilirubin and lecithin.)
The scar tissue that forms in cirrhosis harms the structure of the liver, blocking the flow of blood through the organ.
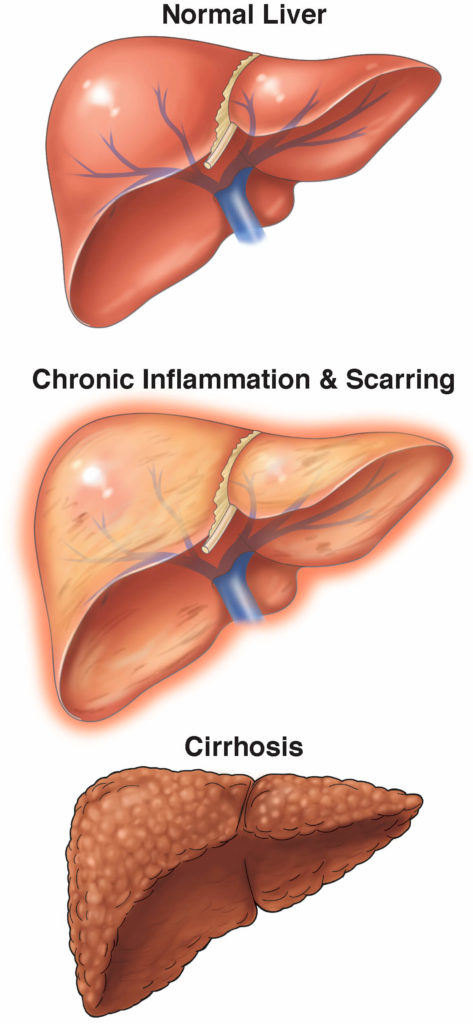
There are many ways to manage advanced cirrhosis:
- Treat the underlying disease.
- Avoid alcohol.
- Practice good nutrition.
- Work closely with a doctor.
- Anticipate and treat complications.
What are the symptoms of cirrhosis?
Patients with cirrhosis often have few symptoms at first.
The two major problems that end up causing symptoms are loss of working liver cells and distortion of the liver caused by scarring.
If you have cirrhosis, you may experience:
-
Extreme tiredness.
-
Weakness.
-
Loss of appetite, often with upset belly and weight loss.
-
Water building up in the legs (edema) or belly (ascites).
-
Easy bruising or bleeding.
-
For females, absent or rare periods not related to menopause.
-
For men, loss of sex drive or tender, enlarged breasts.
What causes cirrhosis?
Cirrhosis has many causes. It can come from certain illnesses or disorders, direct harm to the liver cells, indirect harm by inflammation, or swelling, or a block in the bile ducts, which drain the liver cells of bile.
- Long-term alcohol abuse.
- Chronic viral hepatitis (types B, C and D).
- Nonalcoholic fatty liver disease (NAFLD).
- Autoimmune hepatitis.
- Obesity.
- Inherited (passed down through family) illnesses, such as alpha-1-antitrypsin deficiency, among others.
As the rate of obesity rises, liver disease that may lead to cirrhosis, such as NAFLD and nonalcoholic steatohepatitis (NASH), may become more widespread. These health problems look like alcoholic liver disease, but they happen in people who drink little to no alcohol.
Patients with NAFLD have fatty livers without inflammation or damage, which may not show any symptoms.
NASH involves the buildup of fat in the liver cells, as well as inflammation of the liver, which can kill the liver cells and lead to cirrhosis.
Two inherited illnesses result in the abnormal storage of metals in the liver, leading to tissue damage and cirrhosis.
Wilson’s disease
Patients store too much copper in the liver, brain, kidneys and corneas of the eyes. This is a rare health issue most often seen in children or young adults, not older patients.
Hemochromatosis
Too much iron is taken in by the body, and the extra iron is deposited in the liver and other organs, such as the pancreas, skin, intestinal lining, heart and endocrine glands.
The bile ducts carry bile formed in the liver to the intestines, where the bile helps the body digest fat.
Primary biliary cirrhosis: the liver’s microscopic bile ducts are slowly destroyed.
Primary sclerosing cholangitis: bile ducts inside and outside the liver become swollen and scarred.
Biliary atresia :injury and loss of the bile ducts that are used for draining bile from the liver; found in newborn infants.
Rarely, medications may cause chronic liver disease and cirrhosis. Talk to your doctor about which ones may pose a risk.
There are many causes of cirrhosis that are less often seen, such as veno-occlusive disease, sarcoidosis (granulomatous liver disease), heart failure, and chronic infections, like schistosomiasis and others.
If the cause of cirrhosis is still not clear after a full set of testing, it is termed “cryptogenic cirrhosis.” As many as 10%of patients with cirrhosis fall into this grouping.
Tests for cirrhosis
There are a variety of ways to test for cirrhosis
- Blood tests.
- Imaging studies (CT scan, MRI or ultrasound).
- Physical exam.
- Ultrasound-based transient elastography or MR (magnetic resonance) elastography.
- Noninvasive.
- Measures stiffness of the liver.
- Results can be seen right away.
- Liver biopsy.
- Taking a small piece of tissue from the liver to look at under a microscope.
- Calls for hospitalization for half a day.
- Local numbing is given and medicine to help you relax, if needed.
What’s the treatment for cirrhosis?
Here’s what you can do if you have cirrhosis.
In alcoholic cirrhosis, you must stop drinking alcohol to stop liver damage.
Make sure that you are vaccinated for the flu each year, as well for pneumonia and hepatitis A and B.
Talk to your doctor about any prescription or over the counter medications or supplements you are taking, such as acetaminophen.
Good eating habits are key to the care of advanced cirrhosis.
- Diets that have easy-to-digest forms of protein, such as legumes, poultry and fish, are important.
- A low-salt diet is vital if you have edema (swelling) or ascites (the buildup of fluid in the legs or belly).
- Eat less hard-to-digest proteins, such as red meat, results in fewer toxins in the digestive tract.
- Avoid eating raw seafood, as this may cause severe infections.
Your doctor may recommend medication.
- If you have a certain type of hepatitis, your doctor may give you steroids or antiviral drugs to lessen liver-cell damage.
- If you have edema and ascites, you may be put on a low-salt diet and given diuretics, so that you make more urine to remove fluid and stop the swelling from coming back.
- Medications can control itching.
Liver transplant
Transplant, taking all of a liver from a deceased person or part of liver from a healthy person, is an option for patients with advanced cirrhosis with liver failure. Long-term success rates of liver transplants are good.
Thinking about a transplant requires visits with a team of doctors and lots of testing at a specialty transplant center. Talk to your doctor for more information.
Complications
The main possible problems from cirrhosis are
- Liver failure (when liver cells stop working).
- Bleeding caused by portal hypertension (high blood pressure in the liver). This can often be treated with medications from your doctor.
- Greater risk for liver cancer. The liver should be imaged to screen for liver cancer every six months.
Important facts about medication use
Because the liver may not remove the drugs from the blood as normal, a drug may act longer than called for. This is especially true of sedatives, medications that make you sleepy.



