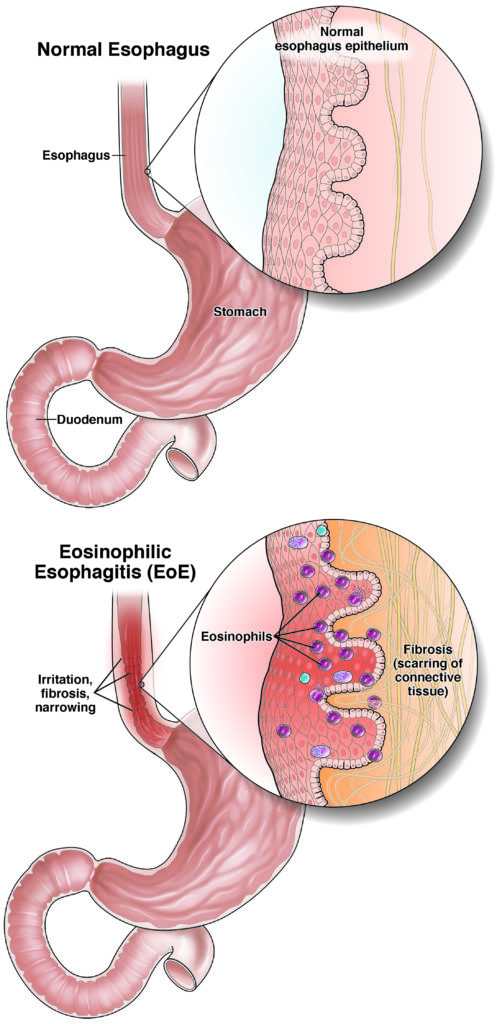
What is eosinophilic esophagitis?
The basics about EoE
Allergy
Many patients with EoE also have food or environmental allergies. People with EoE commonly have other allergic diseases, such as rhinitis, asthma or eczema.
Who gets EoE?
- EoE affects people of all ages and ethnic backgrounds.
- While both males and females may be affected, a higher rate is seen in males.
- Eosinophilic esophagitis is estimated to occur in 1 out of 1,700 people.
- Certain families may have an inherited tendency to develop EoE.
Newly diagnosed with eosinophilic esophagitis
Additional resources
www.apfed.org
Questions to ask your doctor
- How often do I need an endoscopy?
- How do I figure out what’s causing my EoE?
- How long will this last?
- Can my children get this?
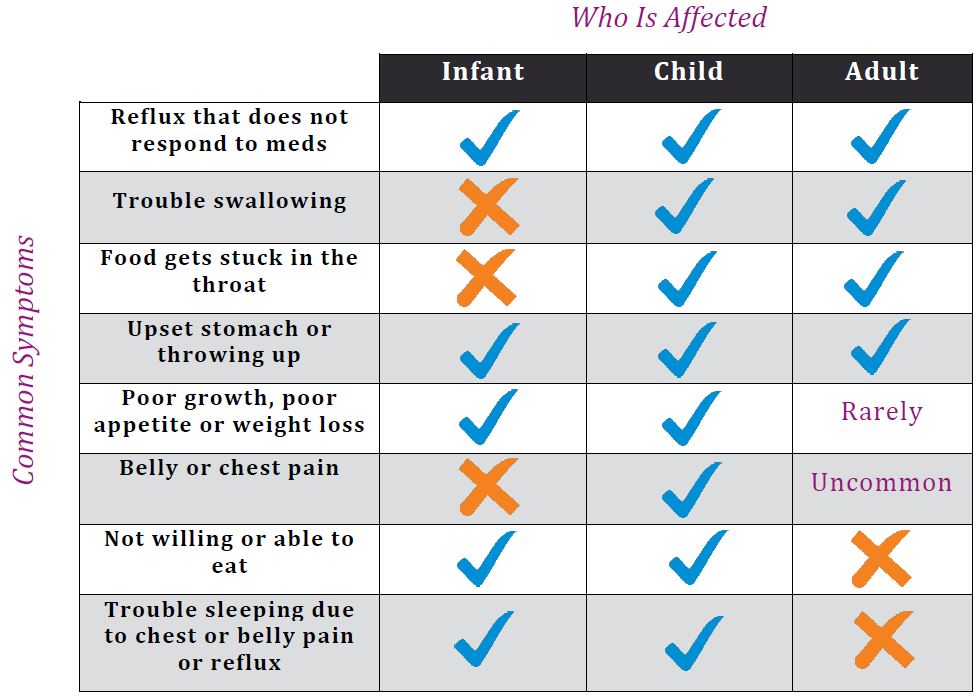
What are the symptoms of eosinophilic esophagitis?
Symptoms of EoE are not the same from one person to the next.
Tests for eosinophilic esophagitis
Finding out you have EoE can only be done by an endoscopy and taking small tissue samples
of the esophagus (the tube that links your mouth and stomach).
Endoscopy
- An endoscopy is done to get a small piece of the tissue (biopsy) from your digestive tract to look at under a microscope to see if there is damage.
- You will be given medicine to help block pain and make you relaxed and sleepy.
- During the endoscopy, your gastroenterologist will use a long, thin (about the width of your little finger), flexible tube with a tiny camera and on the end.
- The tube is passed through the mouth and esophagus into the small intestine as your gastroenterologist does a careful exam.
- Ask your doctor for more information about endoscopy.
Next steps
If your tissue sample says you have EoE
- Your GI doctor will give you information on diet and medicine options.
- Your GI doctor may put you in touch with a registered dietitian (RD) to help you learn more about food tests and elimination diets that could help.
If your tests do not show EoE, some choices your doctor may give you are
- Tracking your symptoms.
- Tracking your diet.
- Considering other tests and medications.
Treatment
There are a few diet options that could help you care for your EoE. Do not start any of these diets unless your doctor or RD tells you to do so:
- Targeted elimination diets: Foods that test positive on allergy testing are removed from the diet.
- Six-food elimination diet: This type of diet has shown success in some patients. Instead of getting rid of foods based on allergy testing results, patients get rid of common allergy-causing foods (milk, eggs, wheat, soy, peanuts/tree nuts, and fish/shellfish).
- Elemental diet: All sources of protein are removed from the diet and the patient drinks only an amino acid formula. Sometimes, a feeding tube may be needed.
- Food trial: Specific foods are removed from the diet and then added back one at a time to figure out which foods cause a reaction.
Diet management involves repeat endoscopies with tissue sample as foods are reintroduced to find out which foods are tolerated.
Some doctors have found these drugs help treat or ease the pain of EoE in certain patients:
- Biologic medicine — A new type of medicine approved by the U.S. Food and Drug Administration (FDA) to treat EoE. Dupilumab is given as an injection and targets certain allergic factors to help stop inflammation. Your doctor can let you know if this medicine is right for you.
- Topical steroids — These are swallowed from an asthma inhaler or a mixture to control EoE.
- Acid suppressors — These may help ease reflux symptoms in some patients in combination with dietary therapy or drugs.
- Proton pump inhibitors (PPIs) — These are most often used for reflux, but can be helpful in EoE.
In some patients, there may be scarring and narrowing of the esophagus (the tube that links your mouth and your stomach) that diet therapy or medications may not treat. As a result, some patients may need to have this area of their esophagus “stretched.”
Esophageal dilation (stretching) can be done at the time of an endoscopy. Often, a balloon is inserted through the flexible tube and then blown up in the area of narrowing to stretch this area open. This can be helpful in relieving the sense of food sticking with swallowing.
Doing this procedure has a small risk that bleeding may occur or a hole could develop in the esophagus (perforation). Rarely, these complications need to be treated with surgery.
Still having symptoms?
It can feel frustrating, or even scary, to keep having symptoms. The first question to think about is: If you are following specific food restrictions or plans, are you consuming the allergen by mistake?
If you are on either a food management plan or drugs, and your symptoms have been there for at least six months, you should speak with your GI doctor about trying both at once to help your EoE symptoms or about other options you may have.
Complications
In some patients, EoE is made worse by the progress of esophageal narrowing (strictures), which may cause food to lodge in the esophagus (the tube that links your mouth and stomach), which is called impaction. This can also make eating very hard and painful for children and adults.

